HYPERCHOLESTERLEMIA
Educational Brochure: HYPERCHOLESTERLEMIA
Instructions:
Design a trifold educational brochure, that will be used to educate the community, about
• HYPERCHOLESTERLEMIA
And
• Pathophysiological factors that influence the incidence and manifestations of acute, episodic, and chronic diseases in populations across the lifespan.
Brochure Contents
1. Two evidenced-based web sites or journal articles as a reference.
2. Risk factors
3. Possible consequences
4. Prevention strategies
5. Treatment modalities
Assignment Requirements:
Before finalizing your work, you should:
• be sure to read the Assignment description carefully (as displayed above);
• consult the Grading Rubric (under the Course Home) to make sure you have included everything necessary; and
• utilize spelling and grammar check to minimize errors.
• follow the conventions of Standard American English (correct grammar, punctuation, etc.);
• be well ordered, logical, and unified, as well as original and insightful;
• display superior content, organization, style, and mechanics; and
• use APA 6th Edition format as outlined in the APA Progression Ladder.
Solution
Educational Brochure: HYPERCHOLESTERLEMIA

Overview
Hypercholesterolemia, conventionally known as dyslipidemia relates to the having higher levels of cholesterol in the blood. As such, this disease is mostly associated with an individual having a high cholesterol level in the blood. According to NHS (2014), cholesterol can be defined as a “soft, waxy, fat-like” material that is a normal or natural constituent of the body cells. Conventionally, our bodies need this cholesterol for the provision of insulation at the nerve myelin sheath to enable effective conveyance of nerve impulses. Also, the liver changes cholesterol to bile to aid intestinal absorption of fats and vitamins. When our bodies generate more cholesterol from the food we eat, it leads to harm. Prevalence of hypercholesterolemia varies depending on its definition. As such, patients with a coronary heart disease have a higher prevalence rate of 80%-88% to developing hypercholesterolemia (Ford, Li, Pearson, Zhao, & Mokdad, 2010). This paper transcends an analysis of hypercholesterolemia focused on educating the public through outlining its risk factors potential strategies to avoid and treat the disorder
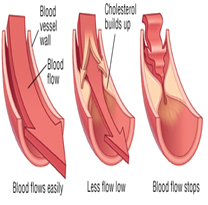
Risk Factors
Hypercholesterolemia can be inherited from parents who have mutated genes that exhibit high levels of low-density lipoprotein in the blood. Additionally, development of hypercholesterolemia can be caused by having a poor diet. Siri-Tarino, Sun, Hu, and Krauss, (2010)suggest that consumption of saturated fat, profoundly found in animals, and other fats contained in commercially produced cookies and crackers raise and individual’s cholesterol levels. Also, obesity, having a BMI of 30+ raises one’s predisposition rates to develop hypercholesterolemia. Furthermore, lack of exercise is another risk factor in developing higher cholesterol levels in the body. It is a proven fact that exercise improves the HDL in the body, “good cholesterol,” as well as increasing the proportions of particles that constitute the LDL(Khera et al., 2011). “bad cholesterol,” making the cholesterol level in the body to be less harmful
Also, smoking and patients who have diabetes have higher chances of developing hypercholesterolemia. Smoking cigarette leads to rapture if the blood vessels which initiates accumulation of deposits of fat in the vessels. Additionally, smoking is associated with lowering the levels of the good cholesterol in the body, leading to a higher percentage of the bad protein. On the other hand, diabetes is characterized by high blood sugar levels which lower the level of HDL cholesterol and increasing the levels of LDL cholesterol. Diabetic patients exhibit high blood sugar are often characterized by the arterial lining damage that can act as deposits of fats. Hence, it can lead to the development of hypercholesterolemia
Last, some medical conditions can predispose an individual to develop hypercholesterolemia. Having a chronic renal insufficiency, hypothyroidism and alcohol dependency can lead to the development of hypercholesterolemia. Also, certain types of medication such as oral estrogens, anti-HIV agents, and atypical antipsychotics can cause mild-moderate levels of hypercholesterolemia
Symptoms of Hypercholesterolemia
Notably, research suggests that at the phases of hypercholesterolemia or high cholesterol there are no physical or visible symptoms(Estoppey, Paccaud, Vollenweider, & Marques-Vidal, 2011). As such, an individual should seek help from a physician in conducting a cholesterol test at the healthcare facility.
Pathophysiological Factors Associated with Hypercholesterolemia
Hypercholesterolemia is triggered by the abnormal metabolism of lipoprotein. This unusual behavior primarily occurs due to a reduction of the LDL receptor activity which reduces the hepatic LDL clearance from the plasma. Consequently, it predisposes an individual to develop atherosclerosis. Also, research suggests that the presence of high cholesterol in the body leads to heart failure and heart attack(Brautbar et al., 2015). Other pathophysiological factors associated with hypercholesterolemia. Includes chronic chest pains and stroke since having this condition alters the functioning of the arteries in the body through the processes of vasoconstriction.
Diagnosis
The only way that a physician can diagnose hypercholesterolemia is by analyzing the results of an individual’s cholesterol levels by the aid of a blood test or lipid profile. The profile depicts the total cholesterol, LDL and HDL cholesterol levels and triglycerides.
Preventive Strategies
Development of hypercholesterolemia can be prevented by the way an individual eats and exercise regularly. Since hypercholesterolemia originates from the trans fatty acids of commercialized food, physicians suggest that individual must have a diet that contains vegetables and fruits. Also, individuals must be engaged in exercises to prevent the development of LDL cholesterol. Undertaking the therapeutic lifestyle changes and Mediterranean-style diet has shown the possibility of reducing the risk of developing hypercholesterolemia.
Treatment of Hypercholesterolemia
There are various medications that one can use to treat high cholesterol levels in the body. First, individuals can utilize the use of statins such as Lovastatin, Pravastatin, and Atorvastatin. These statins help in increasing the levels of HDL cholesterol. Additionally, individuals can use nicotinic acid medication which is used in lowering the levels of LDL cholesterol. The Blue acid sequestrants such as Colestipol, Cholestyramine, and Colesvelam can be used in treating the high levels of the bad cholesterol. Also, patients with hypercholesterolemia are recommended to use nutritional supplements that have less saturated fat, full of whole grains, vegetables, and fruits. Such supplements include fiber that lowers LDL cholesterol levels, Omega-3 fatty acids in fish oil, Vitamin C, and Soy.
References
Brautbar, A., Leary, E., Rasmussen, K., Wilson, D. P., Steiner, R. D., & Virani, S. (2015). Genetics of Familial Hypercholesterolemia. Current Atherosclerosis Reports. https://doi.org/10.1007/s11883-015-0491-z
Estoppey, D., Paccaud, F., Vollenweider, P., & Marques-Vidal, P. (2011). Trends in self-reported prevalence and management of hypertension, hypercholesterolemia and diabetes in Swiss adults, 1997-2007. BMC Public Health, 11, 114. https://doi.org/10.1186/1471-2458-11-114
Ford, E. S., Li, C., Pearson, W. S., Zhao, G., & Mokdad, A. H. (2010). Trends in hypercholesterolemia, treatment and control among United States adults. International Journal of Cardiology, 140(2), 226–235. https://doi.org/10.1016/j.ijcard.2008.11.033
Khera, A. V, Cuchel, M., de la Llera-Moya, M., Rodrigues, A., Burke, M. F., Jafri, K., … Rader, D. J. (2011). Cholesterol efflux capacity, high-density lipoprotein function, and atherosclerosis. The New England Journal of Medicine, 364(2), 127–35. https://doi.org/10.1056/NEJMoa1001689
NHS. (2014). High cholesterol – Diagnosis – NHS Choices. Retrieved from http://www.nhs.uk/Conditions/Cholesterol/Pages/Diagnosis.aspx Siri-Tarino, P. W., Sun, Q., Hu, F. B., & Krauss, R. M. (2010). Saturated fat, carbohydrate, and cardiovascular disease. The American Journal of Clinical Nutrition, 91(3), 502–9.
